Are Shoe Lifts The Best Solution To Leg Length Difference

Leg length inequality goes largely undiagnosed on a daily basis, however this problem is very easily remedied, and can eliminate a number of cases of back discomfort.
Treatment for leg length inequality commonly involves Shoe Lifts . These are very inexpensive, normally priced at below twenty dollars, compared to a custom orthotic of $200 plus. When the amount of leg length inequality begins to exceed half an inch, a whole sole lift is generally the better choice than a heel lift. This prevents the foot from being unnecessarily stressed in an abnormal position.
Upper back pain is the most widespread health problem impacting men and women today. Over 80 million people are affected by back pain at some stage in their life. It is a problem that costs businesses millions of dollars yearly on account of lost time and output. Innovative and more effective treatment solutions are continually sought after in the hope of lowering economical influence this issue causes.

Men and women from all corners of the earth experience foot ache due to leg length discrepancy. In these types of cases Shoe Lifts might be of very helpful. The lifts are capable of alleviating any discomfort and pain in the feet. Shoe Lifts are recommended by numerous skilled orthopaedic orthopedists.
In order to support the human body in a well-balanced fashion, feet have got a significant role to play. In spite of that, it can be the most overlooked zone in the human body. Many people have flat-feet which means there may be unequal force exerted on the feet. This will cause other parts of the body such as knees, ankles and backs to be affected too. Shoe Lifts ensure that proper posture and balance are restored.
Hammer Toe Causes Pain
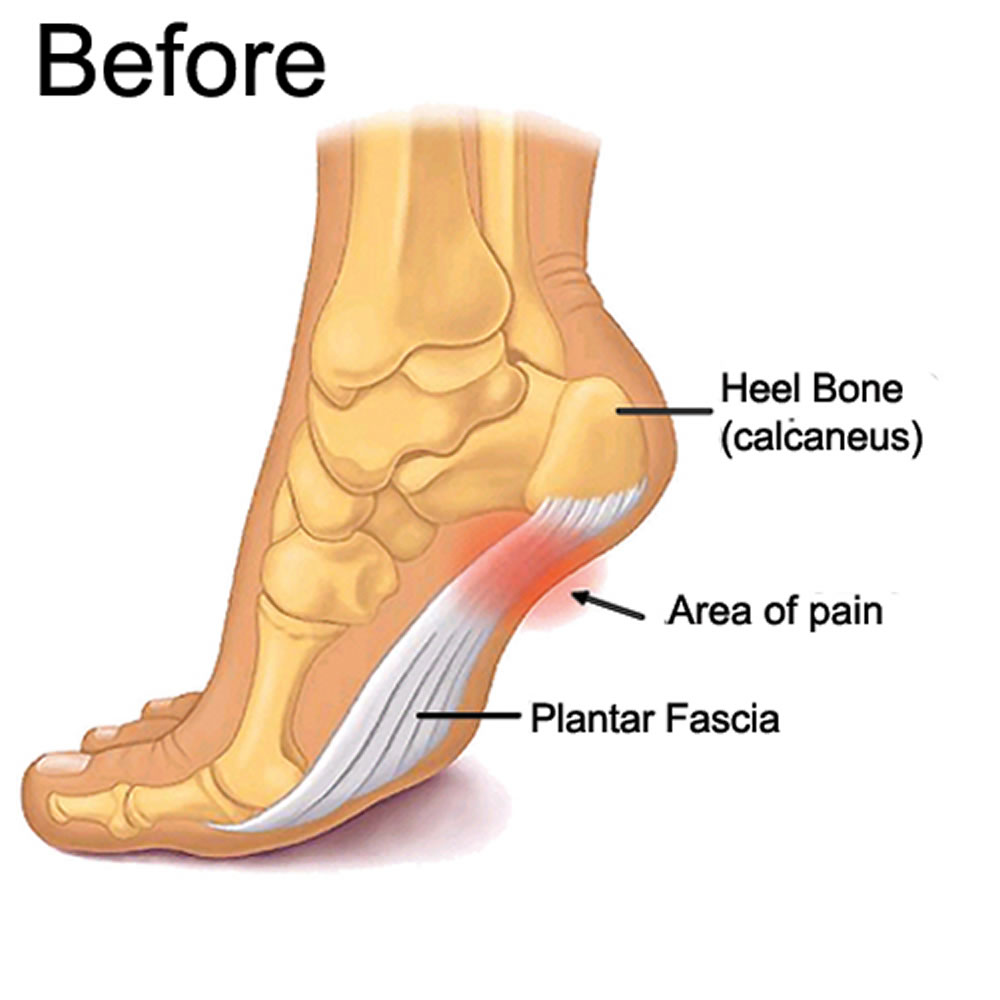 Overview
Overview
There are two types of hammertoe, Flexible hammertoes. If the toe still can be moved at the joint, it's a flexible hammertoe. That's good, because this is an earlier, milder form of the problem. There may be several treatment options. Rigid hammertoes. If the tendons in the toe become rigid, they press the joint out of alignment. At this stage, the toe can't be moved. It usually means that surgery is needed.
Causes
Footwear can contribute significantly to the development of hammertoes. Shoes that are too small force your toes into a curled position. Over time, your toe tendons adjust to this positioning, causing your toe or toes to hold a hammered shape. Athletes may be especially susceptible, because of the increased forces on the toes from shoes that are too small or tight. Heel elevation in footwear is also problematic, as it causes your toes to be pushed into the shoe?s toe box. Heel elevation additionally contributes to muscle imbalance. A common example of this is when your Achilles tendon-the tendon at the back of your leg that attaches your calf muscles to your heel bone-is too tight, causing the tendons on the top of your foot that attach to your toes to work too hard and hold Hammer toe your toes in an unnatural, elevated position.
 Symptoms
Symptoms
People who have painful hammertoes visit their podiatrist because their affected toe is either rubbing on the end their shoe (signaling a contracted flexor tendon), rubbing on the top of their shoe (signaling a contracted extensor tendon), or rubbing on another toe and causing a painful buildup of thick skin, known as a corn.
Diagnosis
Although hammertoes are readily apparent, to arrive at a diagnosis the foot and ankle surgeon will obtain a thorough history of your symptoms and examine your foot. During the physical examination, the doctor may attempt to reproduce your symptoms by manipulating your foot and will study the contractures of the toes. In addition, the foot and ankle surgeon may take x-rays to determine the degree of the deformities and assess any changes that may have occurred.
Non Surgical Treatment
Symptomatic treatment of hammertoes consists of such things as open toed shoes or hammertoe pads. There are over the counter corn removers for temporally reducing the painful callous often seen with the hammertoe. These medications must be used with caution. They are a mild acid that burns the callous off. These medications should never be used for corns or callouses between the toes. Persons with diabetes or bad circulation should never use these products.
Surgical Treatment
Toe Relocation procedures are ancillary procedures that are performed in conjunction with one of the two methods listed about (joint resection or joint mending). When the toe is deformed (buckled) at the ball of the foot, then this joint often needs to be re-positioned along with ligament releases/repair to get the toe straight. A temporary surgical rod is needed to hold the toe aligned while the ligaments mend.
 Prevention
Prevention
Be good to your feet, because they carry you. They are designed to last a lifetime, but that doesn?t mean they don?t need some love and care as well as some basic maintenance. Check your feet regularly for problems. This is especially true if you have diabetes or any other medical condition that causes poor circulation or numbness in your toes. If you do, check your feet every day so problems can be caught early on. Good circulation is essential. When you're sitting down, put your feet up. If you've been sitting for a while, stretch your legs and feet. Give yourself a foot massage, or ask someone you love for a foot massage. A warm foot bath is also a good idea.
Do Bunions Necessitate Surgery
Overview
 Bunions are bony protrusions located at the base of the big toe that develop when the toe is slanted inward or overlaps the next toe. They can be very painful. Bunions form when the movement of the big toe influences the angle of the bones in the foot. The changes gradually develop into the characteristic bump, which over time becomes more and more noticeable.
Bunions are bony protrusions located at the base of the big toe that develop when the toe is slanted inward or overlaps the next toe. They can be very painful. Bunions form when the movement of the big toe influences the angle of the bones in the foot. The changes gradually develop into the characteristic bump, which over time becomes more and more noticeable.
Causes
Heredity and shoe gear are probably the most likely reason for you to develop a bunion. Bunions occur gradually over time. Tight and/or pointy shoes that crowd the toes may result in a bunion. High heels are also suggested to cause bunions as well. See Causes of Bunions.
Symptoms
The symptoms of hallux valgus usually center on the bunion. The bunion is painful. The severe hallux valgus deformity is also distressing to many and becomes a cosmetic problem. Finding appropriate shoe wear can become difficult, especially for women who want to be fashionable but have difficulty tolerating fashionable shoe wear. Finally, increasing deformity begins to displace the second toe upward and may create a situation where the second toe is constantly rubbing on the shoe.
Diagnosis
Clinical findings are usually specific. Acute circumferential intense pain, warmth, swelling, and redness suggest gouty arthritis (see Gout) or infectious arthritis (see Acute Infectious Arthritis), sometimes mandating examination of synovial fluid. If multiple joints are affected, gout or another systemic rheumatic disease should be considered. If clinical diagnosis of osteoarthritic synovitis is equivocal, x-rays are taken. Suggestive findings include joint space narrowing and bony spurs extending from the metatarsal head or sometimes from the base of the proximal phalanx. Periarticular erosions (Martel sign) seen on imaging studies suggest gout.
Non Surgical Treatment
Treatment for bunions ranges from non-surgical to surgical. Conservative, non-surgical treatments are aimed to help alleviate some of the discomfort and pain from the bunion, they will not fix the problem. Some of the recommendations would be shoe modification to make room for the bunion, wearing wide toed shoes, or adding padding and cushioning to your shoes. 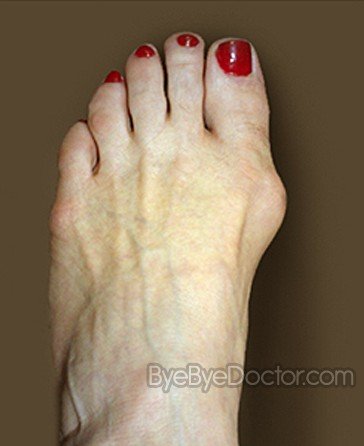
Surgical Treatment
When the pain of a bunion interferes with daily activities, and conservative treatment has been completed it's time to discuss surgical options. Foot Mechanics has excellent relationships with many Orthopaedic Surgeons, who are the specialists who perform bunion surgery. Because bunions are caused by faulty foot mechanics surgery can improve the look of your feet by removing the ?bump? but if the underlying mechanics are not addressed then the bunion is likely to return. For this reason orthotics are used post-surgery to prevent the return of bunions.
Have I Suffered An Achilles Tendon Rupture
Overview
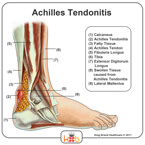 The Achilles tendon is the thickest and strongest tendon in the human body. It plays a very important role in most sport activities and is particularly vulnerable to overloading from repetitive running and jumping. The Achilles tendon forms a joint distal tendon for the gastrocnemius and the soleus muscles. These muscles combine to form the triceps surae muscle. Athletes who sustain Achilles tendon ruptures most frequently are those who participate in ball sports that demand rapid changes of direction and quick, reactive jumps (e.g., tennis, squash, badminton, and soccer), in addition to runners and jumpers in track and field. Sometimes a patient with a ruptured tendon has a history of long-term pain localized to the tendon, but more often the rupture occurs without warning. Such ruptures are often caused by degenerative changes in the tendon (tendinosis), usually in the segment of the tendon that has the worst blood supply. This segment extends from 2 to 6 cm proximal to the insertion of the tendon onto the calcaneus.
The Achilles tendon is the thickest and strongest tendon in the human body. It plays a very important role in most sport activities and is particularly vulnerable to overloading from repetitive running and jumping. The Achilles tendon forms a joint distal tendon for the gastrocnemius and the soleus muscles. These muscles combine to form the triceps surae muscle. Athletes who sustain Achilles tendon ruptures most frequently are those who participate in ball sports that demand rapid changes of direction and quick, reactive jumps (e.g., tennis, squash, badminton, and soccer), in addition to runners and jumpers in track and field. Sometimes a patient with a ruptured tendon has a history of long-term pain localized to the tendon, but more often the rupture occurs without warning. Such ruptures are often caused by degenerative changes in the tendon (tendinosis), usually in the segment of the tendon that has the worst blood supply. This segment extends from 2 to 6 cm proximal to the insertion of the tendon onto the calcaneus.
Causes
As with any muscle or tendon in the body, the Achilles tendon can be torn if there is a high force or stress on it. This can happen with activities which involve a forceful push off with the foot, for example, in football, running, basketball, diving, and tennis. The push off movement uses a strong contraction of the calf muscles which can stress the Achilles tendon too much. The Achilles tendon can also be damaged by injuries such as falls, if the foot is suddenly forced into an upward-pointing position, this movement stretches the tendon. Another possible injury is a deep cut at the back of the ankle, which might go into the tendon. Sometimes the Achilles tendon is weak, making it more prone to rupture. Factors that weaken the Achilles tendon are corticosteroid medication (such as prednisolone), mainly if it is used as long-term treatment rather than a short course. Corticosteroid injection near the Achilles tendon. Certain rare medical conditions, such as Cushing?s syndrome, where the body makes too much of its own corticosteroid hormones. Increasing age. Tendonitis (inflammation) of the Achilles tendon. Other medical conditions which can make the tendon more prone to rupture, for example, rheumatoid arthritis, gout and systemic lupus erythematosus (SLE) - lupus. Certain antibiotic medicines may slightly increase the risk of having an Achilles tendon rupture. These are the quinolone antibiotics such as ciprofloxacin and ofloxacin. The risk of having an Achilles tendon rupture with these antibiotics is actually very low, and mainly applies if you are also taking corticosteroid medication or are over the age of about 60.
Symptoms
Often the person feels a whip-like blow that is followed by weakness in the affected leg - usually he or she is not able to walk afterwards. At place where the tendon ruptured, a significant dent is palpable. Often the experienced physician can diagnose a ruptured Achilles tendon by way of clinical examination and special function tests. Imaging techniques, such as ultrasound and magnetic resonance imaging (MRI) allow for a more precise diagnosis.
Diagnosis
When Achilles tendon injury is suspected, the entire lower lag is examined for swelling, bruising, and tenderness. If there is a full rupture, a gap in the tendon may be noted. Patients will not be able to stand on the toes if there is a complete Achilles tendon rupture. Several tests can be performed to look for Achilles tendon rupture. One of the most widely used tests is called the Thompson test. The patient is asked to lie down on the stomach and the examiner squeezes the calf area. In normal people, this leads to flexion of the foot. With Achilles tendon injury, this movement is not seen.
Non Surgical Treatment
If you suspect a total rupture of the achilles tendon then apply cold therapy and compression and seek medical attention as soon as possible. In most cases surgery is required and the sooner this takes place the higher the chances of success. If the injury is left longer than two days then the chances of a successful outcome decrease. Cold and compression can also be applied throughout the rehabilitation phase as swelling is likely to be an issue with such a serious injury. 
Surgical Treatment
The goal of surgery is to realign the two ends of the ruptured tendon to allow healing. There are multiple techniques to accomplish this goal that will vary from surgeon to surgeon. Recovery from this injury is usually very successful with return to full function in approximately 6 months. Post operatively casting is required with the use of crutches or other means to remain non-weightbearing for 4-8 weeks. This is followed by a course of physical therapy. Partial rupture may or may not require surgical intervention depending on the extent of injury but cast immobilization is a common requirement.